
Concept explainers
Adapting to Host Defenses Surface proteins called HLAs allow white blood cells to detect HIV particles and fight an infection. In a recent study, scientists tested whether HIV is adapting to this host defense. They did so by looking at the frequency of a specific mutation (1135X) in HIV. This “escape mutation” helps the virus avoid detection by a version of the HLA protein (HLA-B*51) that is common in some regions of the world, but not in others. FIGURE 20.19 shows the percentage of HIV-positive people who had HIV with the 1135X mutation. Data were collected at medical centers from several parts of the world.
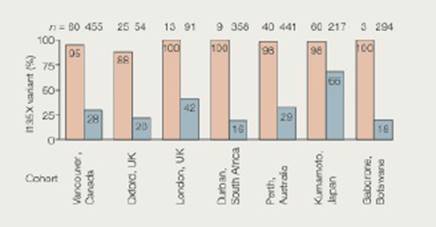
FIGURE 20.19 Regional variation in the frequency of the 1135X escape mutation among HIV-positive people. For each region, pink bars represent the percentage of people whose blood cells have HLA-B*51. and thus cannot detect 1135X mutants. Blue bars represent the percentage of people with other versions of the HLA protein. These people have blood cells that can detect and fight HIV even if it has the 1135X mutation.
4. Japan has a high frequency of HLA-B*51; about half the population has it. How might this explain the high frequency of the 1135X mutation in Japanese with other HLAs?
Want to see the full answer?
Check out a sample textbook solution
Chapter 20 Solutions
Biology: The Unity and Diversity of Life (MindTap Course List)
- picture 1 shows the directed migration of two immune cell types, neutrophils (red) and macrophages (green) to a laser-induced injury in the ear of a mouse. As you can observe from the video, there are three stages to this process: 1) an initial phase characterized by fast recruitment of neutrophils (red) to the site of injury followed by 2) the slower recruitment of macrophages after which 3) the interaction between both cell types is stabilized. Recruitment to the injury site is mediated by leukotriene B4 (LTB4), a potent immune signaling molecule (Figure 1A). LTB4 binds to BLT1, a G-protein coupled receptor (GPCR), activating various signaling pathways and resulting in immune cell migration to the site of injury (Figure 1B). With this background information and your knowledge of cell and molecular biology, describe in detail in your own words, as many molecular processes as you can identify that must take place for the cell migration process depicted in the video to be achieved. For…arrow_forwardWhen the antigen-presenting cells binds to the T-cell, it will cause the T-cell to increase the amount of a protein called perforin, which is secreted to kill nearby cells. Which of these could INCREASE the amount of a functional perforin proteins produced? a. Increased methylation of DNA near the site of the gene b. Increased binding of a repressor, that decreases the binding affinity between TFIID and DNA c. Increased production of a small RNA that is complementary to perforin mRNA d. Increased O-linked glycoslyation of perforin proteins in the Golgiarrow_forwardAdapting to Host Defenses Surface proteins called HLAs allow white blood cells to detect HIV particles and fight an infection. In a recent study, scientists tested whether HIV is adapting to this host defense. They did so by looking at the frequency of a specific mutation (1135X) in HIV. This escape mutation helps the virus avoid detection by a version of the HLA protein (HLA-B51) that is common in some regions of the world, but not in others. FIGURE 20.19 shows the percentage of HIV-positive people who had HIV with the 1135X mutation. Data were collected at medical centers from several parts of the world. FIGURE 20.19 Regional variation in the frequency of the 1135X escape mutation among HIV-positive people. For each region, pink bars represent the percentage of people whose blood cells have HLA-B51. and thus cannot detect 1135X mutants. Blue bars represent the percentage of people with other versions of the HLA protein. These people have blood cells that can detect and fight HIV even if it has the 1135X mutation. 1. What percentage of people with H LA-B51 in Vancouver had HIV with the escape mutation for this protein?arrow_forward
- The Adaptive Immune Response Is a Specific Defense Against Infection In cystic fibrosis gene therapy, scientists propose the use of viral vectors to deliver normal genes to cells in the lungs. What immunological risks are involved in this procedure?arrow_forwardThe Adaptive Immune Response Is a Specific Defense Against Infection Researchers have been having a difficult time developing a vaccine against a certain pathogenic virus as a result of the lack of a weakened strain. They turn to you because of your wide knowledge of recombinant DNA technology and the immune system. How could you vaccinate someone against the virus, using a cloned gene from the virus that encodes a cell-surface protein?arrow_forwardSome viruses have mechanisms to down-regulate MHC class I protein expression on the surface of cells in which the virus is replicating. This immune evasion strategy might prevent effector CD8 cytotoxic T cells from recognizing and killing the virus-infected cells. Would this immune evasion strategy also prevent the initial activation of virus-specific CD8 T cells? Yes, because no viral peptide:MHC class I complexes would form to activate CD8 T cells. No, because dendritic cells would take up infected cells and cross-present viral peptides to activate CD8 T cells. No, because some presentation of MHC class I complexes with viral peptides would occur before the virus could down-regulate all the surface MHC class I protein. Yes, because this immune evasion strategy would also function in dendritic cells, even if the virus doesn’t replicate in dendritic cells. No, because the type I interferon response induced by the virus infection will up-regulate MHC class I expression and override the…arrow_forward
- T cells and B cells have many similarities in how they produce their highly diverse repertoire of antigen receptors, but one important difference between them is that B cell receptors can undergo somatic hypermutation to alter their affinity for antigen. This is known as ‘affinity maturation’, and the result is that the pool of B cells specific for a particular microbe will increase their binding affinity. T cells do not engage in either somatic hypermutation or affinity maturation. Why not? What potential harm could come from allowing T cells to alter the affinity of their TCRs after they have already left the thymus and have become activated in a lymph node or spleen?arrow_forwardSome pathogenic microorganisms encode proteins, such as the Staphylococcus Protein A, that bind to immunoglobulin constant region domains with high affinity. These microbial proteins provide a benefit to the microorganism by: Preventing antibodies bound to the microbe from binding to Fc receptors on phagocytes Blocking the binding of anti-microbial antibodies to the pathogen surface Cleaving the antibody into fragments that separate the antigen-binding region from the effector function Inducing aggregation of the anti-microbial antibodies by multivalent binding to the pathogen-derived protein Preventing the antibody from neutralizing the pathogenarrow_forwardWould it be effective to use an inhibitor of RNA polymerase to block the HIV replication cycle and subsequent infection of human T cells? Yes, this would stop the transcription of viral genes and prevent HIV from being able to replicate. No, these types of inhibitors do not exist and would be impossible to make. No, this would block transcription of T cell genes, leading to the death of T cells and compromised immune systems in individuals. Yes, inhibitors of RNA polymerase are easy and relatively inexpensive to produce and make good therapeutics.arrow_forward
- Which of the following is the most likely explanation for an individual who lacks CCR5 as a result of a homozygous defect in the CCR5 gene becoming infected with HIV? a. The mutated CCR5 genes reverted to the normal form, rendering macrophages susceptible to macrophagetropic HIV variants. b. The macrophage-tropic HIV variant entered host cells using CD4 alone. c. The viral nucleic acid alone was taken up by cells, as in cell transformation by bacterial DNA. d. The individual had received a transplant of HIV-infected cells expressing normal CCR5. e. The primary infection involved a lymphocyte-tropic strain of HIV that used CXCR4 as its co-receptor.arrow_forwardViral DNA in the cytoplasm of a cell can be processed by _________________________, producing a unique dinucleotide ___________________ as a signaling molecule, which can be detected by _____________________. Group of answer choices TLR3 and 2'-5' cyclic AMP (2'-5'cAMP); RIG-I CGas; 2'-5' cyclic GAMP (2'-5' cGAMP); RIG-I TLR3 and 2'-5' cyclic AMP (2'-5'cAMP); CGas CGas; 2'-5' cyclic GAMP (2'-5'cGAMP); STINGarrow_forwardA study is performed in persons with an immunodeficiency disease in which activation of macrophages and B cells by CD4 cells is ineffective. It is observed that all affected persons are males. Laboratory studies show an elevated serum IgM but decreased IgG and IgA. This disorder is most likely to be caused by a mutation in a gene encoding for which of the following? a.CD40 ligand b.Adenine deaminase c.Cytochrome b558 d.Complement C3arrow_forward
 Biology: The Unity and Diversity of Life (MindTap...BiologyISBN:9781305073951Author:Cecie Starr, Ralph Taggart, Christine Evers, Lisa StarrPublisher:Cengage Learning
Biology: The Unity and Diversity of Life (MindTap...BiologyISBN:9781305073951Author:Cecie Starr, Ralph Taggart, Christine Evers, Lisa StarrPublisher:Cengage Learning Human Heredity: Principles and Issues (MindTap Co...BiologyISBN:9781305251052Author:Michael CummingsPublisher:Cengage Learning
Human Heredity: Principles and Issues (MindTap Co...BiologyISBN:9781305251052Author:Michael CummingsPublisher:Cengage Learning Human Physiology: From Cells to Systems (MindTap ...BiologyISBN:9781285866932Author:Lauralee SherwoodPublisher:Cengage Learning
Human Physiology: From Cells to Systems (MindTap ...BiologyISBN:9781285866932Author:Lauralee SherwoodPublisher:Cengage Learning


