
Concept explainers
ABC, health care. Crosstown Health Center runs two programs: drug addict rehabilitation and aftercare (counseling and support of patients after release from a mental hospital). The center’s budget for 2017 follows.
| Professional salaries: | ||
| 4 physicians × $150,000 | $600,000 | |
| 12 psychologists × $75,000 | 900,000 | |
| 16 nurses × $30,000 | 480,000 | $1,980,000 |
| Medical supplies | 242,000 | |
| Rent and clinic maintenance | 138,600 | |
| Administrative costs to manage patient charts, food, laundry | 484,000 | |
| Laboratory services | 92,400 | |
| Total | $2,937,000 |
Kim Yu, the director of the center, is keen on determining the cost of each program. Yu compiles the following data describing employee allocations to individual programs:
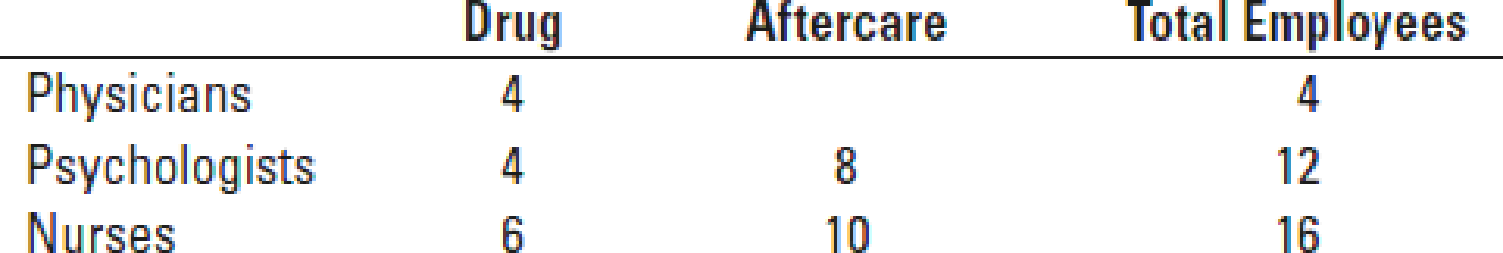
Yu has recently become aware of activity-based costing as a method to refine costing systems. She asks her accountant, Gus Gates, how she should apply this technique. Gates obtains the following budgeted

- a. Selecting cost-allocation bases that you believe are the most appropriate for allocating indirect costs to programs, calculate the budgeted indirect cost rates for medical supplies: rent and clinic maintenance; administrative costs for patient charts, food, and laundry; and laboratory services.
Required
- b. Using an activity-based costing approach to cost analysis, calculate the budgeted cost of each program and the budgeted cost per patient-year of the drug program.
- c. What benefits can Crosstown Health Center obtain by implementing the ABC system?
- 2. What factors, other than cost, do you think Crosstown Health Center should consider in allocating resources to its programs?
Trending nowThis is a popular solution!

Chapter 5 Solutions
REVEL for Horngren's Cost Accounting: A Managerial Emphasis -- Access Card (16th Edition) (What's New in Accounting)
- Meals To Go operates a chain of 10 hospitals in the Los Angeles area. Its central food-catering facility, Mealman, prepares and delivers meals to the hospitals. It has the capacity to deliver up to 1,460,000 meals a year. In 2017, based on estimates from each hospital controller, Mealman budgeted for 1,050,000 meals a year. Budgeted fixed costs in 2017 were $1,533,000. Each hospital was charged $6.16 per meal—$4.70 variable costs plus $1.46 allocated budgeted fixed cost. Recently, the hospitals have been complaining about the quality of Mealman’s meals and their rising costs. In mid-2017, Meals To Go’s president announces that all Meals To Go hospitals and support facilities will be run as profit centers. Hospitals will be free to purchase quality-certified services from outside the system. Dean Wright, Mealman’s controller, is preparing the 2018 budget. He hears that three hospitals have decided to use outside suppliers for their meals, which will reduce the 2018 estimated demand to…arrow_forwardThe hospital where you are employed is continuing with their analysis with the goal of opening a walk-in clinic. After conducting additional research, the financial projections for the first year of operations are as follows: Revenues (from 10,000 visits): $400,000 Wages and benefits: $220,000 Rent: $5,000 Depreciation: $30,000 Utilities: $2,500 Medical supplies: $50,000 Administrative supplies: $10,000 Assume that all costs are fixed except supply costs, which are variable. Assume that the clinic will be required to pay taxes at a 30% tax rate. Respond to the following questions. Be sure to show your work for all calculations. Prepare the clinic’s projected Profit and Loss (P&L) Statement. (8 points) What number of visits is required to break even? (3 points) What number of visits is required to provide you with an after-tax profit of $100,000? (4 points)arrow_forwardBelow are the projected revenues and expenses for a new clinical nurse specialist program being established by a hospital. Nurses would provide education while the patient is in the hospital and home visits after patient discharge on a fee-for-service basis. Should the hospital undertake the program if its required rate of return is 12%? Year 1 Year 2 Year 3 Year 4 Total Revenue costs 100,000 150,000 200,000 250,000 700,000 150,000 150,000 150,000 150,000 600,000 (50,000) 0 50,000 100,000 100,000arrow_forward
- General Hospital, a not-for-profit acute care facility, has the following cost structure for its inpatient services: Fixed costs $1,093,754 Variable cost per inpatient day $19 Charge (revenue) per inpatient day $105 The hospital expects to have a patient load of 1,599 inpatient days next year. Assume that 18 percent of the hospital's inpatient days come from a managed care plan that wants a 27 percent discount from charges. What is the change in profit if the hospital accepts the proposal?arrow_forwardJackson County Senior Services is a nonprofit organization devoted to providing essential services to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: Total Home Nursing Meals On Wheels House-keeping Revenues $ 930,000 $ 267,000 $ 405,000 $ 258,000 Variable expenses 474,000 119,000 198,000 157,000 Contribution margin 456,000 148,000 207,000 101,000 Fixed expenses: Depreciation 69,100 8,300 40,600 20,200 Liability insurance 44,100 20,900 7,800 15,400 Program administrators’ salaries 114,600 40,200 38,400 36,000 General administrative overhead* 186,000 53,400 81,000 51,600 Total fixed expenses 413,800 122,800 167,800 123,200 Net operating income (loss) $ 42,200 $ 25,200 $ 39,200 $ (22,200) *Allocated on the basis of…arrow_forwardJackson County Senior Services is a nonprofit organization devoted to providing essential services to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: Total Home Nursing Meals On Wheels House-keeping Revenues $ 927,000 $ 267,000 $ 402,000 $ 258,000 Variable expenses 465,000 114,000 195,000 156,000 Contribution margin 462,000 153,000 207,000 102,000 Fixed expenses: Depreciation 68,800 8,100 40,400 20,300 Liability insurance 43,200 20,200 7,600 15,400 Program administrators’ salaries 115,400 40,900 38,100 36,400 General administrative overhead* 185,400 53,400 80,400 51,600 Total fixed expenses 412,800 122,600 166,500 123,700 Net operating income (loss) $ 49,200 $ 30,400 $ 40,500 $ (21,700) *Allocated on the basis of…arrow_forward
- Jackson County Senior Services is a nonprofit organization devoted to providing essential services to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: Total Home Nursing Meals On Wheels House-keeping Revenues $ 923,000 $ 265,000 $ 405,000 $ 253,000 Variable expenses 470,000 111,000 202,000 157,000 Contribution margin 453,000 154,000 203,000 96,000 Fixed expenses: Depreciation 69,200 8,200 40,400 20,600 Liability insurance 43,800 20,300 7,600 15,900 Program administrators’ salaries 116,000 40,900 38,200 36,900 General administrative overhead* 184,600 53,000 81,000 50,600 Total fixed expenses 413,600 122,400 167,200 124,000 Net operating income (loss) $ 39,400 $ 31,600 $ 35,800 $ (28,000) *Allocated on the basis of program revenues. The head administrator of Jackson County Senior…arrow_forwardCharity Hospital, a not-for-profit, has a maximum capacity of 15,000 discharges per year. Variable patient service costs are $495 per discharge. Variable general and administrative costs are $5 per discharge. Fixed hospital overhead costs are $4,000,000 per year. The current reimbursement rate is $1,000 per discharge. a. What is Charity’s breakeven volume in number of discharges? b. Now assume Charity’s total discharges for 2014 totaled 10,000. In late 2014, a specialty cardiac hospital opened near Charity, so that discharges in 2015 will reach only 8,500. Management is planning cut fixed costs so that the total for 2015 will be $1,000,000 less than in 2014. Management is also considering reducing variable staffing costs in order to earn a target profit that will be the same dollar amount as the profit earned in 2014. Charity has already had 4,000 discharges in 2015 at a reimbursement rate of $1,000 per discharge with variable costs unchanged. What contribution margin per unit is…arrow_forwardJackson County Senior Services is a nonprofit organization devoted to providing essential services to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: Total Home Nursing Meals On Wheels House-keeping Revenues $ 929,000 $ 266,000 $ 406,000 $ 257,000 Variable expenses 468,000 116,000 196,000 156,000 Contribution margin 461,000 150,000 210,000 101,000 Fixed expenses: Depreciation 69,400 8,400 40,900 20,100 Liability insurance 43,400 20,500 7,400 15,500 Program administrators’ salaries 115,900 40,500 38,600 36,800 General administrative overhead* 185,800 53,200 81,200 51,400 Total fixed expenses 414,500 122,600 168,100 123,800 Net operating income (loss) $ 46,500 $ 27,400 $ 41,900 $ (22,800) *Allocated on the basis of program revenues. The head administrator of Jackson County Senior Services, Judith Miyama, considers last year’s…arrow_forward
- Jackson County Senior Services is a nonprofit organization devoted to providing essential services to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: Total Home Nursing Meals On Wheels House-keeping Revenues $ 919,000 $ 262,000 $ 402,000 $ 255,000 Variable expenses 471,000 112,000 205,000 154,000 Contribution margin 448,000 150,000 197,000 101,000 Fixed expenses: Depreciation 69,700 8,200 40,800 20,700 Liability insurance 43,100 20,100 7,400 15,600 Program administrators’ salaries 116,600 40,900 38,700 37,000 General administrative overhead* 183,800 52,400 80,400 51,000 Total fixed expenses 413,200 121,600 167,300 124,300 Net operating income (loss) $ 34,800 $ 28,400 $ 29,700 $ (23,300) *Allocated on the basis of program revenues. The head administrator of Jackson County Senior…arrow_forwardThe Anacome County Health Department is considering using 300 square feet of excess office space to provide a clinic for Healthchek visits. These visits are reimbursed $75 under a Medicaid program. Variable costs per visit are $45, and providing the service requires an additional physician assistant and nurse with prorated salaries of $85,000 and $65,000 respectively. The state has mandated efforts to increase the utilization of of Medicaid eligibility, so the Department of Social Services is conducting interventions to increase eligibility awareness in the community. As a result, the health department expects 12,000 Healthchek visits in the coming year. Nonavoidable overhead costs for the health department are $300,000 per year and will be allocated to each program based on its proportional share of the health department's total office space of 2,700 square feet. What are the total contribution margin and total product margin for a Healthchek visit? Considering the total…arrow_forwardJackson County Senior Services is a nonprofit organization devoted to providing essential ser-vices to seniors who live in their own homes within the Jackson County area. Three services are provided for seniors—home nursing, Meals On Wheels, and housekeeping. Data on revenue and expenses for the past year follow: The head administrator of Jackson County Senior Services, Judith Miyama, is concerned about the organization’s finances and considers the net operating income of $5,000 last year to be razor-thin. (Last year’s results were very similar to the results for previous years and are representative of what would be expected in the future.) She feels that the organization should be building its financial reserves at a more rapid rate in order to prepare for the next inevitable recession. After seeing the above report, Ms. Miyama asked for more information about the financial advisability of perhaps discontinuing the housekeeping program. The depreciation in housekeeping is for a…arrow_forward
 Cornerstones of Cost Management (Cornerstones Ser...AccountingISBN:9781305970663Author:Don R. Hansen, Maryanne M. MowenPublisher:Cengage Learning
Cornerstones of Cost Management (Cornerstones Ser...AccountingISBN:9781305970663Author:Don R. Hansen, Maryanne M. MowenPublisher:Cengage Learning Managerial Accounting: The Cornerstone of Busines...AccountingISBN:9781337115773Author:Maryanne M. Mowen, Don R. Hansen, Dan L. HeitgerPublisher:Cengage Learning
Managerial Accounting: The Cornerstone of Busines...AccountingISBN:9781337115773Author:Maryanne M. Mowen, Don R. Hansen, Dan L. HeitgerPublisher:Cengage Learning Managerial AccountingAccountingISBN:9781337912020Author:Carl Warren, Ph.d. Cma William B. TaylerPublisher:South-Western College Pub
Managerial AccountingAccountingISBN:9781337912020Author:Carl Warren, Ph.d. Cma William B. TaylerPublisher:South-Western College Pub


