
Concept explainers
Adapting to Host Defenses Surface proteins called HLAs allow white blood cells to detect HIV particles and fight an infection. In a recent study, scientists tested whether HIV is adapting to this host defense. They did so by looking at the frequency of a specific mutation (1135X) in HIV. This “escape mutation” helps the virus avoid detection by a version of the HLA protein (HLA-B*51) that is common in some regions of the world, but not in others. FIGURE 20.19 shows the percentage of HIV-positive people who had HIV with the 1135X mutation. Data were collected at medical centers from several parts of the world.
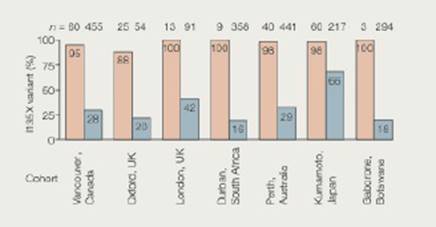
FIGURE 20.19 Regional variation in the frequency of the 1135X escape mutation among HIV-positive people. For each region, pink bars represent the percentage of people whose blood cells have HLA-B*51. and thus cannot detect 1135X mutants. Blue bars represent the percentage of people with other versions of the HLA protein. These people have blood cells that can detect and fight HIV even if it has the 1135X mutation.
1. What percentage of people with H LA-B*51 in Vancouver had HIV with the escape mutation for this protein?
Want to see the full answer?
Check out a sample textbook solution
Chapter 20 Solutions
Biology: The Unity and Diversity of Life (MindTap Course List)
- picture 1 shows the directed migration of two immune cell types, neutrophils (red) and macrophages (green) to a laser-induced injury in the ear of a mouse. As you can observe from the video, there are three stages to this process: 1) an initial phase characterized by fast recruitment of neutrophils (red) to the site of injury followed by 2) the slower recruitment of macrophages after which 3) the interaction between both cell types is stabilized. Recruitment to the injury site is mediated by leukotriene B4 (LTB4), a potent immune signaling molecule (Figure 1A). LTB4 binds to BLT1, a G-protein coupled receptor (GPCR), activating various signaling pathways and resulting in immune cell migration to the site of injury (Figure 1B). With this background information and your knowledge of cell and molecular biology, describe in detail in your own words, as many molecular processes as you can identify that must take place for the cell migration process depicted in the video to be achieved. For…arrow_forwardOne strategy for vaccine development currently under investigation is the use of pathogen-derived T cell epitopes as a component of the vaccine. For viral pathogens, implementing this strategy involves scanning the predicted amino acid sequences of the viral proteins for likely peptide epitopes that would bind to MHC class I and MHC class II molecules. In addition to the complication of MHC sequence polymorphism in the human population, another complication of this strategy for peptide epitopes that would bind to MHC class II proteins is: The importance of viral proteins containing peptides that are cleaved into 8–10 amino acid long fragments. The ability of viruses to mutate their proteins to avoid MHC anchor residue sequences. The fact that long peptides (>13 amino acids) are rapidly degraded in cells. The fact that MHC class II proteins are intrinsically stable, even in the absence of binding to a peptide. The absence of defined sequence motifs that predict peptide binding to…arrow_forwardIn addition to phagocytosis, neutrophils use a process called NETs. Which one of the following describes this process? Group of answer choices A. NETs is a neutrophil process that activates the complement system of proteins, which destroys pathogens. B. A net-like structure of DNA, histones, lactoferrins, gelatinase, cathepsin G, and myeloperoxidase is secreted at pathogens. Together these chemicals destroy pathogens. C. NETs works when neutrophils secrete major basic proteins onto pathogens, destroying the pathogens' cell membranes. D. NETs are chemicals secreted by neutrophils that trigger the rapid maturation of lymphoid stem cells into lymphocytes.arrow_forward
- We now have at least three SARS-CoV-2/COVID-19 vaccines approved by the FDA for use in the United States. These vaccines cause cells in the body to make the spike protein that is on the surface of the virus, and subsequently, stimulate an antibody response to this antigen. A. What do these antibodies do to prevent infection by SARS-CoV-2? How do they interact with the virus particles? B. Which kind of cells in the immune system are responsible for synthesizing these antibodies?arrow_forwardSome Pattern Recognition Receptors (PRRs) recognize nucleic acids, like RNA or DNA. Since our own cells contain human RNA and DNA, the activation of innate immune pathways by these PRRs must rely on additional criteria to discriminate self from nonself. Additional criteria include everything EXCEPT: The subcellular location of the RNA The presence of adenosine residues in viral RNA The methylation state of the DNA Unique structures found on viral RNA The subcellular location of the DNAarrow_forwardA study is performed in persons with an immunodeficiency disease in which activation of macrophages and B cells by CD4 cells is ineffective. It is observed that all affected persons are males. Laboratory studies show an elevated serum IgM but decreased IgG and IgA. This disorder is most likely to be caused by a mutation in a gene encoding for which of the following? a.CD40 ligand b.Adenine deaminase c.Cytochrome b558 d.Complement C3arrow_forward
- Some viruses have mechanisms to down-regulate MHC class I protein expression on the surface of cells in which the virus is replicating. This immune evasion strategy might prevent effector CD8 cytotoxic T cells from recognizing and killing the virus-infected cells. Would this immune evasion strategy also prevent the initial activation of virus-specific CD8 T cells? Yes, because no viral peptide:MHC class I complexes would form to activate CD8 T cells. No, because dendritic cells would take up infected cells and cross-present viral peptides to activate CD8 T cells. No, because some presentation of MHC class I complexes with viral peptides would occur before the virus could down-regulate all the surface MHC class I protein. Yes, because this immune evasion strategy would also function in dendritic cells, even if the virus doesn’t replicate in dendritic cells. No, because the type I interferon response induced by the virus infection will up-regulate MHC class I expression and override the…arrow_forwardSuppose you have two A-B-type exotoxins, A-B and A’-B’. A-B binds specifically to all MHC-II cells and blocks vesicle trafficking. A’-B’ binds specifically to all MHC-I cells and stops protein synthesis. a. What would a hybrid toxin, A’-B, do to fibroblast (skin) cells? Provide your rationale. b. What would a hybrid toxin, A-B’, do to fibroblasts? Provide your rationale. c. What would a hybrid toxin, A’-B, do to macrophages? Provide your rationale. d. What would a hybrid toxin, A-B’, do to macrophages? Provide your rationale.arrow_forwardThe immunoglobulin molecules of a particular mammalian species have kappa and lambda light chains and heavy chains. The kappa gene consists of 250 V and 8 J segments. The lambda gene contains 200 V and 4 J segments. The gene for the heavy chain consists of 300 V, 8 J, and 4 D segments. If just somatic recombination and random combinations of light and heavy chains are taken into consideration, how many different types of antibodies can be produced by this species?arrow_forward
- Can you compare and contrast the infection process of influenza and HIV? What are the specific molecules on the surface of each virus that directly interacts with the respective cellular receptor molecule? What is/are the specific molecules on the surface of the respective target cells that serve as the cellular receptors for these viruses respectively?arrow_forwardAccording to the article which was written before the COVID-19 vaccine was created, when do people turn to magic? How can this tendency, which happens across cultures and throughout history, contribute to the current spread of the novel coronavirus and its variants?arrow_forwardWhen an antibody binds to the spike protein of SARS-CoV-2, it may block access of the spike protein to the ACE2 protein on human cells. This is one way an antibody can prevent the virus from attaching to and getting inside of human cells. But antibodies can do more than just block virus entry. Due to the symmetrical structure of the immunoglobulin molecule, it can bind to two antigen molecules simultaneously, like this: As a result, antibodies can cross-link multiple viruses in a three-dimensional network. Using this diagram as a starting point, draw several additional viruses and antibodies to illustrate what a cross-linked antigen-antibody complex might look like.arrow_forward
 Biology: The Unity and Diversity of Life (MindTap...BiologyISBN:9781305073951Author:Cecie Starr, Ralph Taggart, Christine Evers, Lisa StarrPublisher:Cengage LearningEssentials of Pharmacology for Health ProfessionsNursingISBN:9781305441620Author:WOODROWPublisher:Cengage
Biology: The Unity and Diversity of Life (MindTap...BiologyISBN:9781305073951Author:Cecie Starr, Ralph Taggart, Christine Evers, Lisa StarrPublisher:Cengage LearningEssentials of Pharmacology for Health ProfessionsNursingISBN:9781305441620Author:WOODROWPublisher:Cengage Human Heredity: Principles and Issues (MindTap Co...BiologyISBN:9781305251052Author:Michael CummingsPublisher:Cengage Learning
Human Heredity: Principles and Issues (MindTap Co...BiologyISBN:9781305251052Author:Michael CummingsPublisher:Cengage Learning Human Physiology: From Cells to Systems (MindTap ...BiologyISBN:9781285866932Author:Lauralee SherwoodPublisher:Cengage Learning
Human Physiology: From Cells to Systems (MindTap ...BiologyISBN:9781285866932Author:Lauralee SherwoodPublisher:Cengage Learning Human Biology (MindTap Course List)BiologyISBN:9781305112100Author:Cecie Starr, Beverly McMillanPublisher:Cengage Learning
Human Biology (MindTap Course List)BiologyISBN:9781305112100Author:Cecie Starr, Beverly McMillanPublisher:Cengage Learning





